Arthritis of the ankle joint is a chronic disease that affects the articular cartilage, and subsequently other joint structures (capsule, synovium, bone, ligament). It has a degenerative-dystrophic character. It manifests itself as pain and limitation of movement, followed by progressive deterioration of support function and walking. Diagnosis is made based on symptoms, examination and radiography. Treatment is usually conservative, using anti-inflammatory drugs, chondroprotectors and glucocorticoids, and prescribing exercise therapy and physical therapy. In severe cases, hygienic arthroscopy, arthrodesis or endoprosthetics are performed.
General information
Osteoarthritis of the ankle joint is a disease in which the articular cartilage and surrounding tissue are gradually destroyed. This disease is based on a degenerative-dystrophic process; inflammation in the joint is secondary. Arthrosis has a chronic wave-like course with alternating remissions and exacerbations, and gradually develops. Women and men suffer equally often. The likelihood of development increases dramatically with age. At the same time, experts note that the disease is "getting younger" - every third case of ankle arthrosis is now detected in people under the age of 45.
Cause
Primary arthrosis occurs for no apparent reason. Secondary damage to the ankle joint develops under the influence of several unfavorable factors. In both cases, the basis is a violation of metabolic processes in cartilage tissue. The main causes and predisposing factors for the formation of secondary arthrosis of the ankle joint are:
- major intra- and periarticular injuries (talus fractures, ankle fractures, ligament tears and ruptures);
- ankle surgery;
- overload: too intense sports, long walks or continuous standing due to work conditions;
- wearing shoes with heels, overweight, constant microtrauma;
- diseases and conditions related to metabolic disorders (diabetes mellitus, gout, pseudogout, estrogen deficiency during menopause);
- rheumatic disease (SLE, rheumatoid arthritis);
- osteochondrosis of the lumbar spine, intervertebral hernia and other conditions accompanied by pinched nerves and disorders of the muscular system of the legs and feet.
Less common, causes of arthrosis are non-specific purulent arthritis, arthritis due to specific infections (tuberculosis, syphilis) and congenital developmental anomalies. Unfavorable environmental conditions and hereditary tendencies play a certain role in the development of arthrosis.
Pathogenesis
Normally, the articular surfaces are smooth, elastic, slide smoothly relative to each other during movement and provide effective shock absorption under load. As a result of mechanical damage (trauma) or metabolic disorders, cartilage loses its smoothness, becoming rough and inelastic. Cartilage "rubs" during movement and injures each other, which leads to worsening pathological changes.
Due to insufficient depreciation, excess load is transferred to the underlying bone structure, and degenerative-dystrophic disorders also develop in it: the bone changes shape and grows along the edges of the articular area. Due to secondary trauma and normal biomechanical disorders of the joint, not only the cartilage and bone suffer, but also the surrounding tissue.
The joint capsule and synovial membrane are thickened, and foci of fibrous degeneration are formed in the periarticular ligaments and muscles. The joint's ability to participate in movement and bear the load is reduced. Instability occurs and pain develops. In severe cases, the articular surface is destroyed, the supporting function of the limb is impaired, and movement becomes impossible.
symptoms
At first, rapid fatigue and mild pain in the ankle joint are detected after a significant load. After that, the pain syndrome becomes more intense, the nature and time of occurrence changes. The characteristic features of pain with arthrosis are:
- Start pain. Appears after a state of rest, and then gradually disappears with movement.
- Dependence on load. There is increased pain during exercise (standing, walking) and rapid joint fatigue.
- Night pain. Usually appears in the morning.
The situation changes in waves, during exacerbation the symptoms are more pronounced, in the phase of remission they first disappear, then become less intense. There is a gradual development of symptoms over years or decades. Along with pain, the following manifestations are determined:
- When moving, a pulsating, squeaking or clicking sound may occur.
- During an exacerbation, the periarticular area sometimes swells and becomes red.
- Due to the instability of the joint, the patient often twists his leg, causing sprains and tears in the ligaments.
- Stiffness and range of motion are noted.
Complications
During exacerbation, reactive synovitis may occur, accompanied by fluid accumulation in the joint. At the next stage, significant deformations are revealed. Movement is severely restricted and contractures develop. Support becomes difficult; when moving, the patient had to use crutches or crutches. There is a decrease or loss of ability to work.
Diagnostics
The diagnosis of arthrosis of the ankle joint is made by an orthopedic doctor based on a survey, external examination data and the results of additional studies. When examined at the initial stage, there may be no changes, but later deformation, limitation of movement, and pain on palpation are revealed. The main importance is given to visualization techniques:
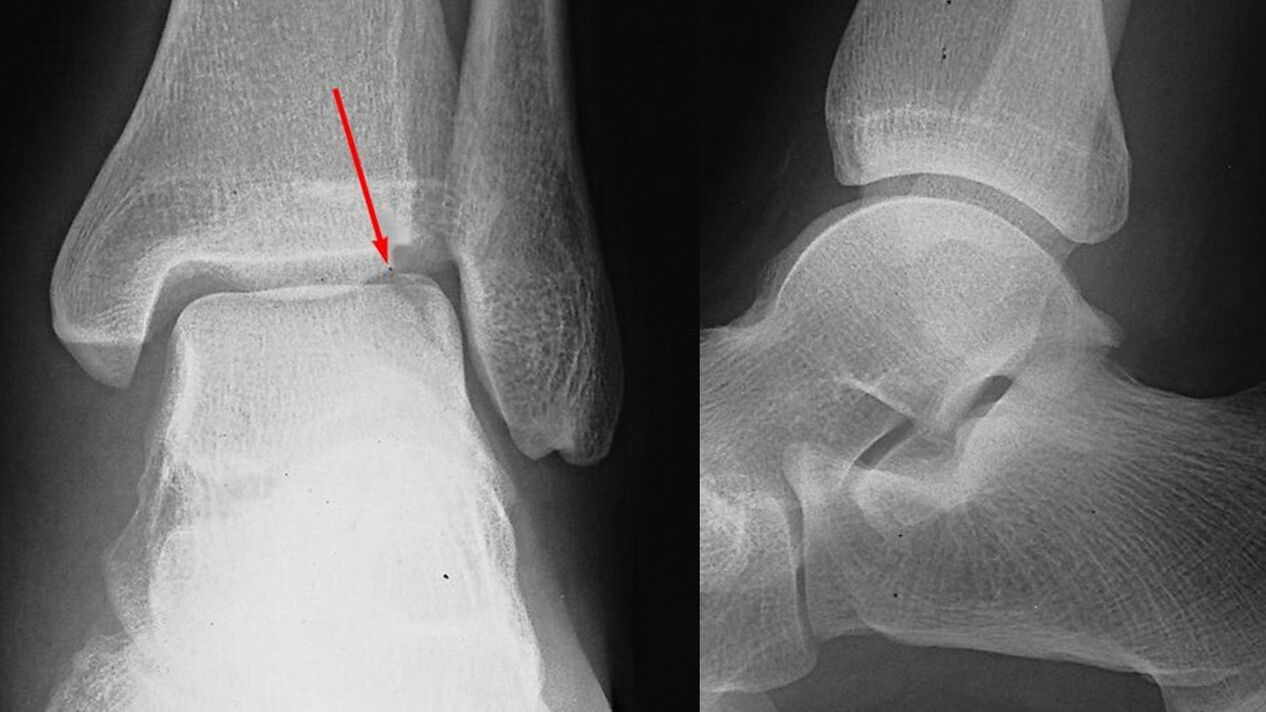
- X-ray of the ankle joint. Plays an important role in making a diagnosis and determining the degree of arthrosis. Pathology is manifested by narrowing of the joint space, proliferation of the edges of the articular surface (osteophytes). At the next stage, the formation of cysts and osteosclerosis of the subchondral zone (located under the cartilage) of the bone is detected.
- Tomographic study. Used when indicated. In difficult cases, for a more accurate assessment of the state of the bone structure, the patient is also sent to a computed tomography scan, and to examine the soft tissues - to an MRI of the ankle joint.
Laboratory tests were unchanged. If necessary, to establish the cause of arthrosis and differential diagnosis with other diseases, consultation with relevant specialists is prescribed: neurologist, rheumatologist, endocrinologist.
Treatment of ankle arthrosis
Pathological treatment is long-term and complex. Patients are usually seen by orthopedic surgeons on an outpatient basis. During the period of exacerbation, hospitalization in traumatology and orthopedic departments is possible. The most important role in slowing down the development of arthrosis is played by the correct lifestyle and mode of physical activity, therefore patients are given recommendations to lose weight and optimize the load on the legs.
Drug therapy
It is selected individually, taking into account the stage of arthrosis, the severity of symptoms and concomitant diseases. Including general and local agents. The following groups of drugs are used:
- General NSAIDs. Usually tablet form is used. Medicines have a negative effect on the gastric mucosa, so for gastrointestinal diseases, "gentle" medicines are better.
- Topical NSAIDs. Recommended during periods of exacerbation and in the phase of remission. Can be prescribed as an alternative if side effects from the tablet form occur. Available in the form of ointment and gel.
- Chondroprotectors. A substance that helps normalize metabolic processes in cartilage tissue. They are used in the form of creams, gels and preparations for intra-articular administration. Use a medicine that contains glucosamine and collagen hydrolyzate.
- Hormonal agents. In cases of severe pain that cannot be relieved by medication, intra-articular corticosteroids are given no more than 4 times a year.
- Metabolic stimulant. To improve local blood circulation and activate tissue metabolism, nicotinic acid is prescribed.
Physiotherapy treatment
The patient is prescribed a complex of physical therapy, developed taking into account the manifestation and stage of the disease. The patient was referred for physiotherapy. In the treatment of arthrosis, massage and UHF are used. In addition, in the treatment of pathology they use:
- laser therapy;
- thermal procedures;
- medical electrophoresis and ultraphonophoresis.
Surgery
Shown in the final stages of the disease when conservative therapy is ineffective, severe pain syndrome, deterioration in the patient's quality of life, or limited ability to work. The operation is carried out in a hospital environment and is open and minimally invasive:
- Arthroscopic Intervention. If there is significant cartilage destruction, arthroscopic chondroplasty is performed. Sanitary arthroscopy (removal of formations that prevent movement) is usually performed for severe pain in stage 2 arthrosis. The effect lasts for several years.
- Arthrodesis of the ankle joint. It is performed in case of significant destruction of the articular surface, involving the removal of the joint and "fusion" of the leg and lower leg bones. Provides restoration of limb support function in case of loss of joint mobility.
- Ankle joint endoprosthetics. Performed for advanced arthrosis. Involves removing the articular surface of the destroyed bone and replacing it with a plastic, ceramic or metal prosthesis. Movement is fully restored, the service life of the prosthesis is 20-25 years.
Prediction
Changes in the joints are irreversible, but the slow development of arthrosis, the timely start of treatment and compliance with the recommendations of orthopedic traumatologists in most cases make it possible to maintain the ability to work and a high quality of life for decades after the appearance. from the first symptoms. With the rapid increase in pathological changes, endoprosthetics allow a person to avoid deformities.
Prevention
Preventive measures include reducing the level of injuries, especially in winter, during the ice period. If you are obese, it is necessary to take steps to lose weight to reduce the load on the joints. You should maintain a moderate physical activity regime, avoid overloading and microtraumas, and immediately treat diseases that can trigger the development of arthrosis of the ankle joint.



































